It is no secret that healthcare professionals work in a high-pressure environment, being subjected to intense work schedules and demands from not just patients themselves, but also from the patients’ families.
Maintaining staff wellbeing has therefore been a long-time effort of Singapore’s National Healthcare Group (NHG), which manages care needs in the country’s central region. And this task is no small one, either, considering how the NHG has 22,000-plus staff under its wing.

So, from previously focusing on a “triple aim” of improving the patient experience, delivering better health outcomes, and lowering the cost of care, the NHG has since expanded the goal to include a fourth aim: enhancing the staff experience.
“Staff wellbeing has always been on our mind, especially [since] we are a healthcare organisation,” says Adjunct Associate Professor Yong Keng Kwang, Group Chief Nurse and Chief Wellness Officer of the NHG.
At Intellect’s recent Mental Health Festival 2023, Prof Yong shares four strategies the NHG has put in place to foster organisational wellbeing and provide timely person-centred support across its seven healthcare institutions.
Watch the replay here:
1. Balancing psychological safety and accountability
The NHG promotes a culture of shared governance—namely, a culture of shared decision-making, shared accountability, and staff-leader collaboration.
In Prof Yong’s words, doing so “dilut[es] the power gradient”, breaks down communication barriers, and helps staff feel psychologically safe to provide feedback on improving patient safety and care.
“We want to give nurses at all levels a voice to make sure that they can raise any issues [on their mind],” says Prof Yong.
At Yishun Health, for example, the institution adopts a Speaking Up for Safety (SUFS) programme where healthcare staff are taught how to use a Safety C.O.D.E. of Checks, Options, Demands, and Elevates to raise patient care concerns with colleagues in a respectful yet progressively decisive way.

“Being at the forefront of clinical care, they need to [be able to] escalate the matter to people who can deal with the issue,” he says.
Speaking up, however, is only half of it; taking action is the other. The use of an online Promoting Professional Accountability tool also helps enforce professional accountability throughout the organisation.
Staff can use the tool to submit confidential positive and negative feedback about their peers’ work conduct. A triage team then reviews the submissions to decide whether to have a Peer Messenger discuss the matter with the named staff over a “cup of coffee”.
2. Managing internal stressors
Apart from dealing with external stressors such as patient abuse, healthcare staff may also face internal stressors that hinder their ability to provide quality patient care.
For example, a staff may become involved in, or have contributed to, an incident where a patient under their care suffered harm. Even though the staff had not been the direct victim in the incident, they may still experience distress over it—especially if the harm had not been intentionally caused.
In these situations, the staff inadvertently becomes the incident’s “second victim”. And if their trauma goes undetected and unmanaged, they may suffer in silence to the point that they can no longer perform their work well.
The NHG hence implements a Second Victim Support Framework to provide three levels of support to second victims, starting with Mental Health First Aid™ and progressing to professional counselling and guidance, to help the affected staff bounce back from the incident.
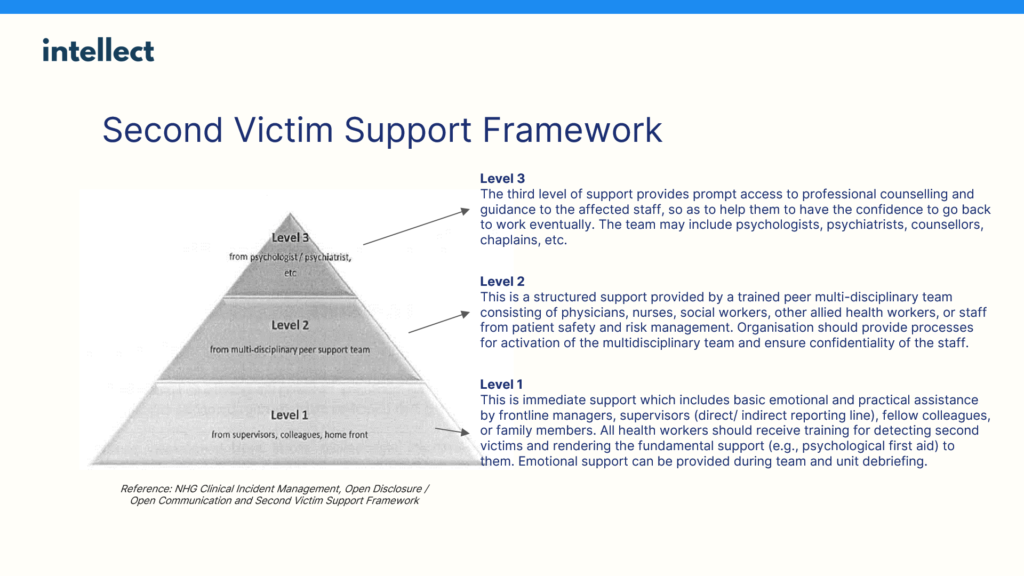
Being a victim of workplace harassment, abuse, or bullying can be another source of internal stress. Acknowledging the detrimental impact that bullying can have on mental health, the NHG trains its staff to recognise potential incidents of workplace bullying. It also equips staff with practices for responding to and reporting the incident to nip it in the bud.

3. Setting fresh graduates and leaders up for success
Healthcare is a people-intensive industry, and the worsening nursing resignation rates have not helped: Prof Yong shares that these rates for calendar years 2021 and 2022 were “at least 50% higher” compared to that for calendar year 2019—before the COVID-19 pandemic hit.
The NHG therefore has to deploy its talent pool effectively to continue providing high-quality patient care, notwithstanding its limited resources.
When recruiting fresh graduates, the NHG is mindful that the work they are expected to perform may not fully align with what they had been taught in school, given the increasingly “complex” nature of healthcare.
The NHG is thus putting in more effort to match these first-jobbers with suitable roles, and reduce the culture shock and workplace anxiety they may experience during the transition.
And while the NHG previously placed a “high emphasis” on competence, its current leadership development programme focuses more on cultivating traits relating to building relationships, fostering engagement, and empowering others to do their best work.

“We look at promoting leaders who are able to facilitate an environment for people to interact openly,” shares Prof Yong.
4. Taking a tiered approach to care
There is no one-size-fits-all approach to maintaining and improving mental health. Accordingly, the NHG employs different measures to care for its staff’s wellbeing across the mental health continuum. This is not unlike Intellect’s philosophy to mental healthcare and Singapore’s national mental health and wellbeing strategy.
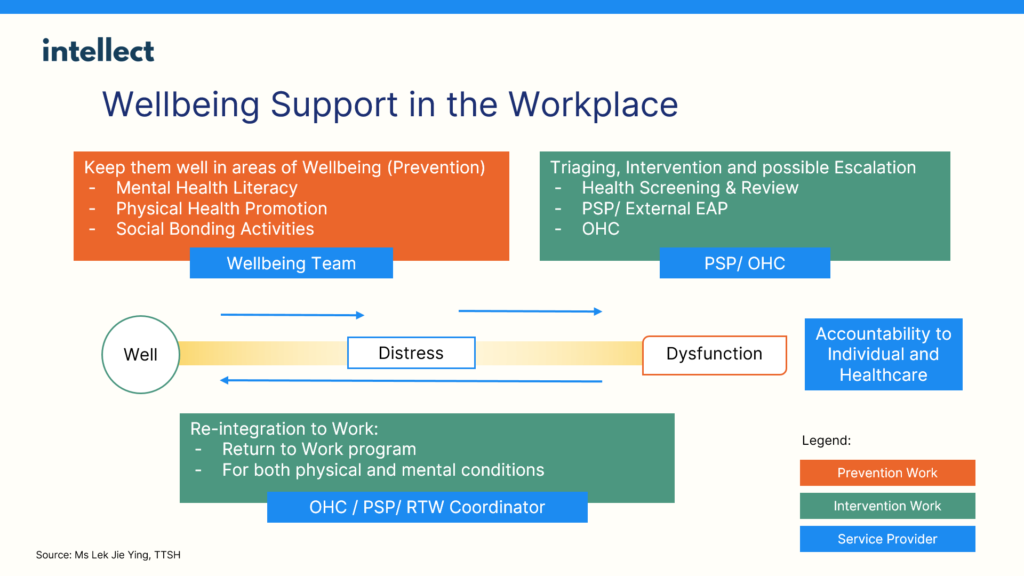
For example, wellbeing support at Tan Tock Seng Hospital involves supporting the physical and mental wellbeing of staff across three stages of “Well”, “Distress”, and “Dysfunction”.
The hospital aims to keep staff “Well” by implementing preventive measures such as increasing mental health literacy and promoting the importance of maintaining physical health.
However, if it detects instances of staff experiencing “Distress” or “Dysfunction”, it triages the situation to decide whether to intervene or even escalate it. The actions taken at these stages could include activating its Peer Support Programme (PSP) or an external Employment Assistance Programme (EAP).
“EAP services complement our Peer Support Programme because they offer neutral, third-party support for staff who prefer anonymity. And hopefully, that will help our staff overcome any barriers to seeking help,” says Prof Yong.
Destigmatising mental health at work
Intellect offers a range of services catering to all needs across the mental health continuum. These include:
1. Mental Health First Aid™, of which Intellect is the sole licensed provider in Singapore. It empowers individuals, especially wellbeing ambassadors, to recognise when their peers are experiencing mental distress and direct them towards appropriate avenues for help.
2. Intellect EAP with a 24/7 helpline and EAP concierge manned by qualified responders who can provide in-the-moment support and de-escalate critical situations. It also offers Critical Incident Stress Management support to organisations in high-risk situations.
3. Access to mental healthcare professionals including coaches, counsellors, and clinical psychologists in over 20 countries. Sessions may be conducted virtually or in person at our clinics at Tanjong Pagar and Parkway MediCentre in The Woodleigh Mall.
Book a demo here to learn how your people and business can benefit from Intellect.






